 
The skin area where insertion is to take place constitutes the most important source of CVC infection. 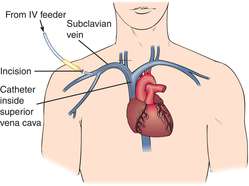
Use the maximum universal aseptic measures in the implant by maintaining all possible protective and safety barriers for the environment and handling. Keep adequate hygiene of the hands by washing them with soap and water or with alcohol-based gel, maintaining aseptic techniques for any handling of the CVC. Conservative treatment without withdrawing the catheter is acceptable for tunnelled catheters infected by the customary microorganisms: i) associated systemic antibiotic therapy should be administered ii) intraluminal sealing of the catheter with suitable antibiotics: iii) intraluminal sealing with antibiotics not associated with systemic therapy is ineffective. In cases of severe infection or when the catheter is not withdrawn, empiric antibiotic therapy should be set in motion prior to reception of microbiological test results. Extractions should be simultaneous and cultivated using quantitative techniques whenever possible. If a patient with CVC presents fever, blood cultures of peripheral blood from both branches of the catheter should be extracted. 
If there is septic shock, bacteraemia with hemodynamic decompensation or tunnelitis with fever, the catheter should be immediately removed. However, most of the other aspects can be regarded as institutional (place, insertion method, catheter material, care in handling, etc), and it is precisely these factors that have an important bearing on reducing infection. There are factors that depend on the patient such as the existence of an underlying illness, immune system compromise, serious illness, comorbidity, etc. Impregnation of catheter with antisepticsĬharacteristics of patient Underlying illness and immune system compromise Reed et al, has described all the variables that play a part in CVC complications in a microbiological and ultrastructural study. Experts consider that current standards for pump flow (Qb), venous pressure (Pv), molecular clearance and dialysis time could be improved and reductions in clinical complications can be reduced by enhancements in the process, thereby increasing the quality of life for patients and reducing the health care costs caused by this problem. Vascular access dysfunction causes the highest consumption of resources in the population with chronic kidney disease (CKD). When the density of microorganisms reaches a certain level, the probability of catheter related sepsis increases considerably. The germs are usually immersed in a biofilm sticking to the interior and exterior of the catheter formed by the interaction of the catheter wall with host proteins.Īppearance of the film is very early, even in the first 24 hours after insertion, but is not necessarily a determining factor in the appearance of infection. Studies using electron microscopes show that the immense majority of catheters, even those where the quantitative culture gives negative results, are colonised by microorganisms. More is starting to be known about the mechanism through which CVC contamination is produced thanks to the development of experimental models with animals. The incidence of infection attributable to catheter use varies amongst hospitals and is about 4-5 events per 1000 days of catheterisation, and an average mortality of 3% is linked to this sizeable prevalence. 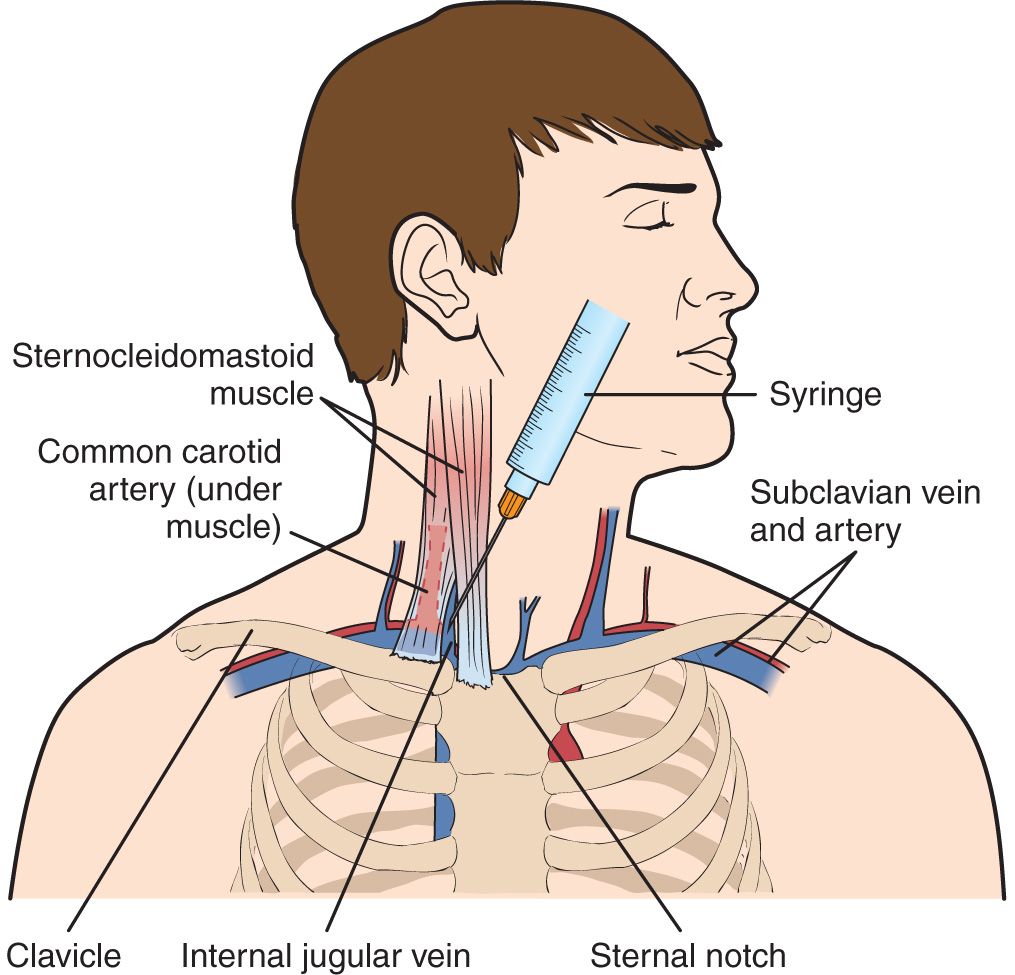
Infection from use of central vascular catheters (CVC) constitutes one of the main complications and the main cause of primary nosocomial bloodstream infection. However, they are not exempt from risks such as infectious or mechanical complications arising from their use. These devices have been of great clinical use as they enable fast, safe access to the bloodstream to administer medications, treatments fluids and parenteral nutrition. Intravascular catheters are plastic devices that provide access to the intravascular compartment at a central level, they vary in design and structure according to if they are temporary (days) or permanent (weeks, months) as well as in the material they are made of and the reason why they are implanted. Ideal VA should bring together at least three requirements: i) a safe, continuous approach to the vascular system ii) provision of sufficient flow to supply an adequate HD dosage, and iii) present no complications. The need for vascular access is as old as HD itself, given that access to the bloodstream is necessary to eliminate toxic substances. The complications arising from VA dysfunction constitute one of the main causes of morbidity and mortality amongst patients and substantially increase health care costs. The quality of vascular access (VA) is a determining factor in clinical results of patients receiving periodic haemodialysis treatment (HD). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
